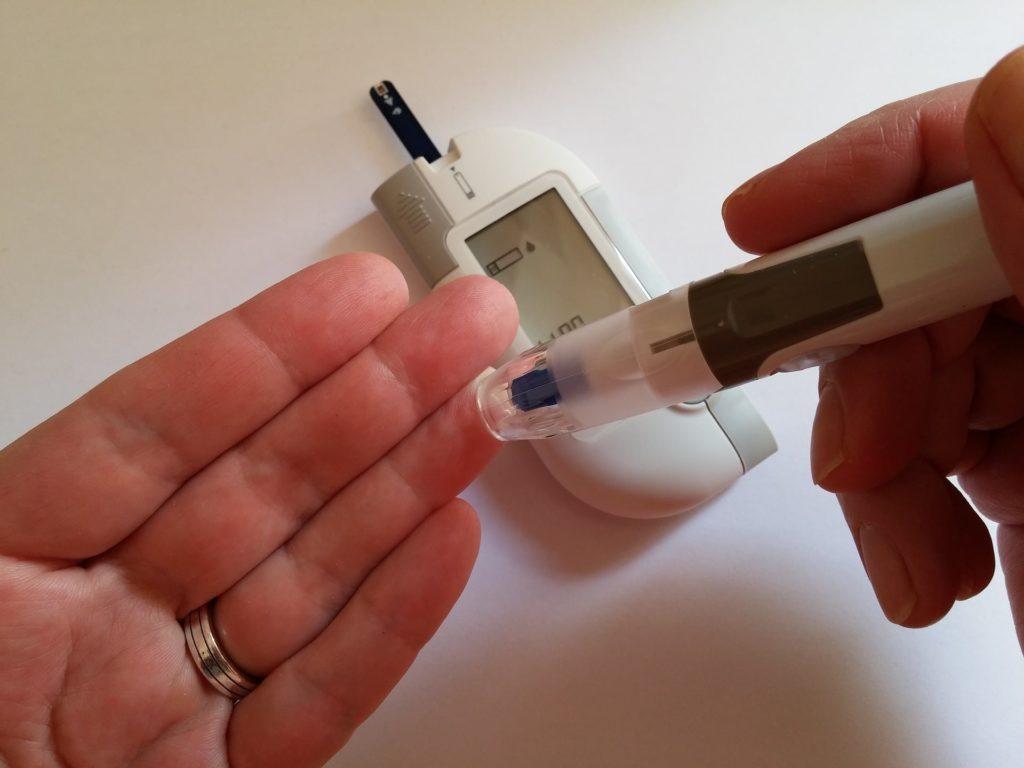
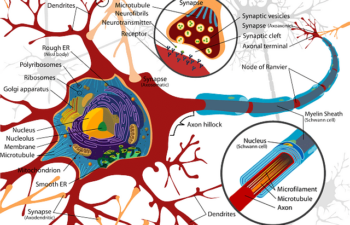
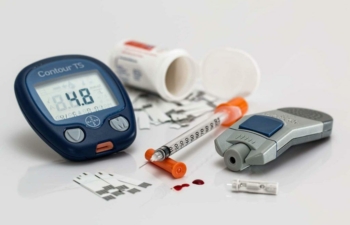
Diabetes is a disorder of sugar metabolism that affects almost every organ system in the human body. In humans, our nervous system can be divided into the central and peripheral nervous systems. The central nervous system is our brain and cranial nerves. Peripheral nervous system is the other all the peripheral nerves.
Peripheral nervous system can be divided into few sub-categories according to the function of nerves as sensory (sensations), motor (actions) and autonomic (actions of unconscious). Neuropathy is a medical term for any disease of the nerves. When the disease is caused by diabetes, it is called diabetic neuropathy. Diabetes affects almost all nerves in the body, but the effects are more pronounced in the peripheral nervous system. Therefore, diabetic peripheral neuropathy can be sensory, motor or autonomic. Each has its own signs and symptoms.
Medical definition
The medical definition of diabetic peripheral neuropathy is the presence of symptoms and/or signs of peripheral nerve dysfunction in people with diabetes, after exclusion of other causes of neuropathy. Neuropathy is the most common complication of uncontrolled or long-standing diabetes. With inadequate glycaemic control, neuropathy can develop in almost 75% of patients within 2 years, in both type 1 and type 2 diabetes mellitus.
The main symptom of diabetic neuropathy is altered sensation of the skin. In most cases it is reduced sensation, but in a few cases the sensation can become painful. Reduced sensation can lead to secondary signs and symptoms such as foot and skin ulcers, falls, burns, cuts and secondary infections, which can even lead to limb amputation or death.
Clinically, diabetic peripheral neuropathy can be divided into a few stages based on signs and symptoms.
- Chronic painful diabetic peripheral neuropathy
- Burning, shooting, stabbing pains associated with pins and needle sensations
- Pain increased at night
- Absent sensation to several modalities such as temperature, touch, pain
- Reduced or absent reflexes
- Acute painful diabetic peripheral neuropathy
- Severe symptoms as chronic painful
- May be associated with start of the insulin in poorly controlled diabetics
- Painless with complete or partial sensory loss due to diabetic peripheral neuropathy
- Severe numbness injuries
- Reduced temperature sensations
- Absent reflexes
- Late complications of diabetic peripheral neuropathy
- Foot ulcers and deformities
- Non-traumatic amputation
- Dead limbs
Risk
In general, 30% of people with diabetes have peripheral neuropathy at the time of diagnosis. In the USA, it is estimated that 3 – 5% of diabetics develop neuropathy-associated serious complications such as amputations and even death. Worldwide, 40-50% of non-traumatic amputations are due to diabetic neuropathy.
Assessment
Neuropathy is assessed clinically. Ideally, this should be done annually. The main reason is to identify the predominant neuropathy and to identify risk factors and warning signs for the development of neuropathy in the near future.
History
A detailed medical history should be part of the diabetes risk assessment. This should include the following:
- Age
- Sex
- Nationality
- Type of diabetes
- Medications
- Alcohol and smoking status
- Employment
- Leisure activities
- Use of foot wear or special footwear
- Mobility
- Home circumstances
- Social support
- Access to health care facilities
- Knowledge about diabetes and neuropathy
Examination of the feet
Remove your shoes and socks, then wash your feet with lukewarm water and wipe them with a clean towel. Your feet should be checked for the following:
- Skin – color, consistency ,thickness, dryness , cracks, sweat
- Interdigital areas – fungal infections, ulcers
- Calluses
- Blisters
- Deformities
- Foot arches
- Sensation to pain, touch, temperature
- Should palpate for sensory and pulses such as dorsalis pedis artery and posterior tibial artery.
- Check capillary refill time (CRFT)
- Nails for their color and consistency
Neurological assessment of the foot
This is the most important test and should be done at least every 2 months. It is a very simple test requiring only a 10g monofilament and a good light source. The feet are palpated with the monofilament and the patient rates the sensation. If the patient can't feel it, the test is positive for diabetic peripheral neuropathy.
Other types of diabetic peripheral neuropathy
Autonomic diabetic peripheral neuropathy
When the autonomic nerves are affected by diabetes, it is called autonomic diabetic peripheral neuropathy. Autonomic nerves supply all the internal organs such as the heart, lungs, intestines, reproductive organs and other internal organs. When there is autonomic diabetic peripheral neuropathy, the function of these organs is affected and can lead to different disorders specific to each organ.
Examples:
- Heart – arrhythmias, palpitations and increased fatigue
- Gut – ileus, gut motion dysfunctions
Motor diabetic peripheral neuropathy
Motor means “action”. Actions in our body are mainly carried out by the musculoskeletal system. Motor nerves supply the musculoskeletal system. Every muscle in the body has its own nerve. When diabetic peripheral neuropathy affects the nerve, the muscle is also affected. This results in reduced function and loss of muscle fibres.
Summary
Diabetic peripheral neuropathy is the most common complication of diabetes. It can lead to various complications such as ulcers, amputations and even death. Early detection and treatment reduce the risks.