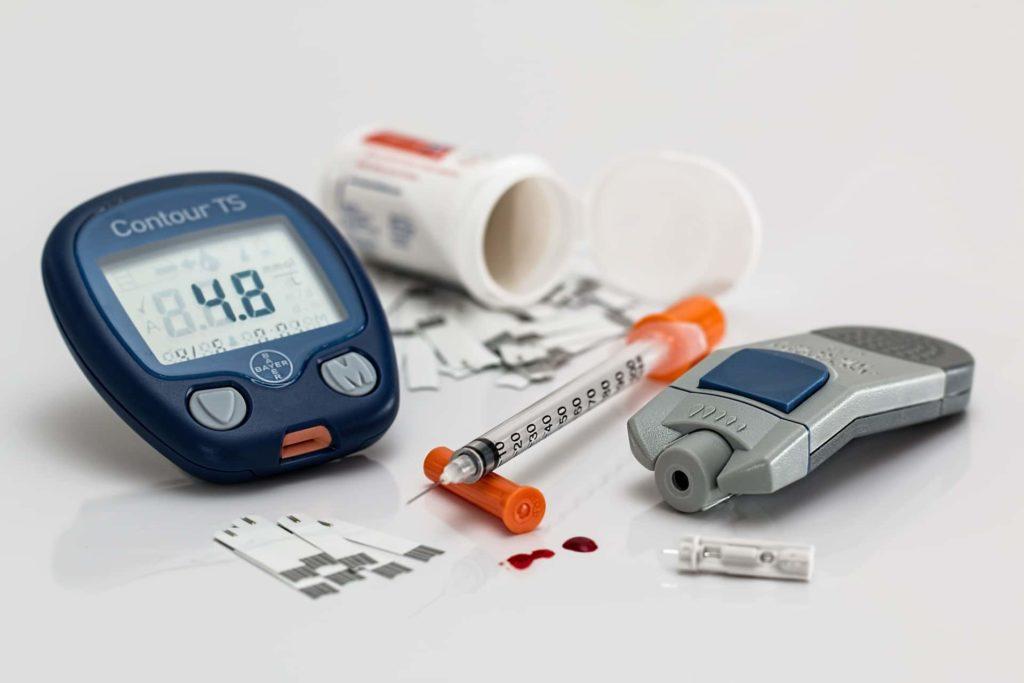
Diabetes is a disorder of glucose metabolism that affects almost every organ system in the human body. Neuropathy is the most common complication of uncontrolled or long-standing diabetes. With inadequate glycaemic control, up to 75% of patients may develop neuropathy within 2 years, in both type 1 and type 2 diabetes mellitus.
The pathogenesis or medical pathophysiology of diabetic peripheral neuropathy is a complex process. There are many theories about its pathophysiology. Most scientists agree that it is multifactorial or that there are many factors that contribute to the development of diabetic peripheral neuropathy. The most important factor is the presence of persistent and uncontrolled hyperglycaemia.
Persistent hyperglycemia
Like any other tissue in the human body, nerves are made up of cells. The nerve cells are called neurons. Neurons also depend on oxygen and glucose for their survival. Glucose metabolism, combined with oxygen, provides energy for neurons to function and survive. If the neurons are functioning properly, then the whole unit, the nerve, is functioning well. A change in this function is the disease of the nerves, i.e. neuropathy.
Prolonged hyperglycaemia increases the sugar metabolism pathways in the peripheral nerves, which in turn increases the sugar levels inside the nerve cells. In particular, sugars such as sorbitol and fructose accumulate inside the nerve cells and damage them. This damage results in reduced enzyme activity inside the neuron, which leads to the accumulation of various ions inside the neuron, such as sodium. When sodium accumulates inside, it draws water into the cells and causes the cell to swell. This swelling causes cell damage, which is usually irreversible. It causes nerve degeneration and therefore neuropathy.
Immune Mechanisms
Immune mechanisms involving the different types of white blood cells and other chemicals released by the white blood cells and the human immune system may be responsible for diabetic peripheral neuropathy. In general, our immune system produces various chemicals such as antibodies and cytokines to destroy harmful microbes and other harmful cells such as cancer cells. But in people with diabetes mellitus, their nerve cells are known to be coated with chemicals that signal the immune system to attack them. The white blood cells, antibodies and various other chemicals then attack and destroy the nerve cells. This leads to nerve degeneration and diabetic peripheral neuropathy.
Chronic micro-vascular ischemia
Chronic microvascular ischaemia or insufficiency or lack of blood supply to the nerves is another process that occurs in diabetic peripheral neuropathy. Nerves have small blood vessels that supply them with blood. These blood vessels are called vasa nervorum. They run long with the nerves. They have a very small calibre and are easily blocked. Blockage of the blood vessels is mainly caused by thickening of the vessel walls. Hyperglycaemia is when the blood sugar level is higher than normal. This causes sugar or glucose to bind to various blood cells and other proteins in the blood. After binding, glucose forms various complexes with the bound products. These products are heavy and as they circulate through the vessels they tend to deposit along the wall, causing the wall to thicken. Thickening of the wall causes the lumen of the blood vessel to become narrow.
When the lumen of the blood vessel becomes narrowed, the circulation of blood is reduced and causes a lack of nutrients and glucose to the nerves. This leads to nerve damage and nerve degeneration, resulting in diabetic peripheral neuropathy. It has been found that 95% of chronic diabetics have long-term nerve ischaemia.
Growth Factor Deficiency
Growth factor deficiency is another proven cause of diabetic peripheral neuropathy. Growth factors are essential for the growth, maintenance, survival and regeneration of nerves. Nerves are damaged on a daily basis by various mechanisms. Growth factors are essential for the repair process and a lack of them can lead to irreversible damage and nerve degeneration.
Mechanism of pain in diabetic peripheral neuropathy
Pain is one of the most serious consequences of diabetic peripheral neuropathy. It significantly reduces activities of daily living and quality of life. Pain is an unpleasant sensation that our brain detects in many noxious stimuli. Stimuli are transmitted via the nerves and if the neuronal circuitry is not functioning properly, it can lead to false stimuli and cause various pain syndromes. Additionally, don't miss out on the variety of neuropathy products at our online store.
The causes of many pain syndromes are varied and the pathology can be found in different parts of the peripheral nervous system. This can include nerve branches, nerve terminals, axons, synapses, the spinal cord and associated nerve tracts, and peripheral neuronal ganglia. These carry the messages to the pain centre and activate the pain. It is more pronounced in patients with uncontrolled, long-term severe hyperglycaemia. There are many treatments for pain, but the mainstay remains good glycaemic control.